Keep vibing for life by taming chronic inflammation
As we age, our bodies subtly change. Aches and pains become more commonplace, our movements might lack their youthful spring, and our eyesight might even lose some clarity. But what if there is a way to slow down this process, to feel younger and more energetic for longer? The answer could lie in understanding and managing a hidden culprit: chronic inflammation.
What is inflammation?
Inflammation is your body’s way of protecting itself when something harmful happens, such as an injury, infection or irritation. It’s a biological alarm that goes off to signal that something’s wrong. When your body detects a threat, like bacteria, viruses or toxins, it sends out immune cells, like white blood cells, to fight the problem and help you heal.
When you notice signs of inflammation, like redness, swelling, heat, pain or difficulty moving the affected area, your first thought should be that this is your body’s way of showing that it’s working hard to heal you. However, when it is severe or persistent, then it can spell trouble.
While acute inflammation is a necessary and beneficial process that helps the body fight off infections and heal injuries, chronic inflammation can be harmful. Chronic inflammation occurs when inflammation sticks around for too long, often due to underlying health conditions such as autoimmune diseases, obesity or long-term exposure to irritants like pollution and cigarette smoke.

The connection between inflammation and ageing
Inflammageing is a specific type of chronic, low-grade inflammation that develops with age. It’s different from the acute inflammation you experience with a cut or infection because it happens in the absence of any obvious cause.
Cellular decline
Persistent activation of the immune system damages healthy tissues instead of just fighting off invaders. One way this happens is through cellular senescence. Our cells naturally slow down as we age, but inflammageing can accelerate this process. These dysfunctional cells accumulate and hinder tissue repair, contributing to wrinkles, muscle weakness and organ decline.
Weakened immune system
The constant low-grade ‘slow-burning fire’ of inflammageing can confuse the immune system. It becomes less effective at fighting off actual infections and diseases, making seniors more susceptible to illness.
Organ damage
Continually elevated inflammation levels can damage vital organs like the heart, lungs and brain. This increased stress is a major risk factor for age-related diseases such as heart disease, diabetes, cancer and neurodegenerative disorders like Alzheimer’s.
We’ve discussed how chronic inflammation is linked to ageing. Now, you might be surprised to learn how our oral health significantly impacts this process. Our mouths, especially when affected by periodontal (gum) disease, can become a breeding ground for inflammation.
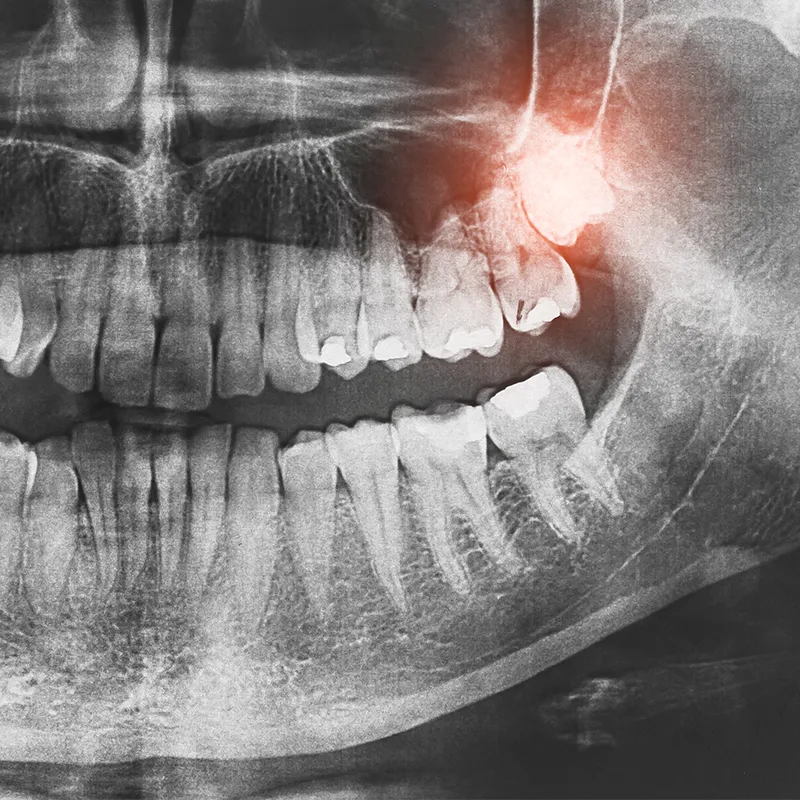
Periodontal disease is a chronic inflammatory condition. It affects the tissues supporting our teeth, including the gums, periodontal ligament (fibres connecting teeth to bone) and jawbone. When plaque and bacteria build up along the gumline, they trigger an immune response, leading to inflammation and tissue damage.
Left untreated, periodontal disease can progress, causing tooth loss and increasing the risk of systemic inflammation. Furthermore, the harmful bacteria from these oral infections aren’t confined to the mouth. They can enter the bloodstream, triggering inflammation throughout the body. This systemic inflammation can then exacerbate the ageing process and contribute to the development of other age-related conditions.

Fight inflammation and stay younger with healthy habits
Thankfully, we can turn down the flames of inflammation and promote healthy ageing through mindful lifestyle choices.
Brush away bad bacteria: Excellent oral hygiene is your first line of defence. Brushing twice daily, flossing regularly and visiting your dentist keep your mouth healthy and inflammation at bay.
Move your body: Regular exercise is a potent anti-inflammatory weapon. Get your body moving and reap the benefits of improved overall health and reduced inflammation.
Stress less, live more: Chronic stress fuels the fire. Find healthy ways to manage stress, like yoga, meditation or spending time in nature. You’ll be amazed at how much better you feel!
Sleep and recharge: Aim for 7-8 hours of quality sleep each night. When you’re sleep-deprived, your body struggles to fight inflammation. Prioritise sleep for optimal health and a more energetic you.
Fuel your body right: Go for a whole-food, anti-inflammatory diet rich in fruits, vegetables and healthy fats (e.g., nuts & fish). Limit processed foods, sugar and unhealthy fats.

You’re in control!
Inflammation is a natural part of ageing, but don’t give it the final say on how you experience your adulthood. Through smart lifestyle choices, prioritising oral health and collaborating with your healthcare team, you can help keep this internal fire stay under control and experience a healthier, more vibrant life, no matter your age.
Remember, gaining understanding is only your first step toward living your best life. Consult your dentist and doctor for personalised advice on managing inflammation and thriving with outstanding health.