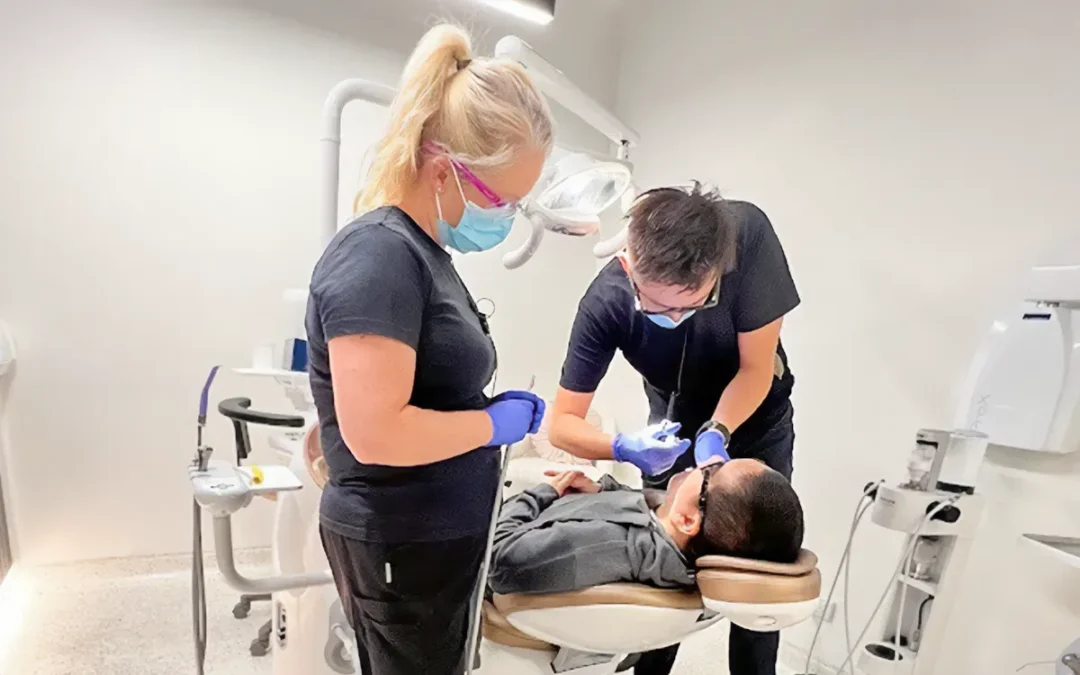
Professional dental hygiene appointments in 8 steps
You’ve circled the date, and now it’s here. Time for your dental hygiene appointment. But what really happens once you’re in that chair?
It’s easy to think of these visits as just a minor clean to tick off your to-do list if time allows. In reality, they’re one of the most powerful tools for protecting your smile and your health. Far beyond a surface polish, a professional dental hygiene appointment is a deep dive into your mouth’s well-being. This is your pro-level frontline defence against decay, gum disease, and more.
In our calm and comfortable treatment room, your dental team checks for early signs of issues you can’t see or feel yet, removes stubborn buildup that even the best toothbrush can’t handle, and tailors advice to help you keep your teeth strong for life.
Curious or even a bit anxious? Understanding what happens during your visit helps you appreciate the care and science behind it. Each appointment does more than clean your teeth. It helps maintain your long-term health.
Why bother with professional dental hygiene appointments?
Brushing and flossing at home are essential, but they’re not enough on their own. No matter how meticulous your daily routine is, plaque can still accumulate in areas your toothbrush and floss can’t reach. Over time, this plaque hardens into tartar, which can only be removed with specialised periodontal tools like an ultrasonic scaler or Airflow. That’s where your dental hygienist comes in.
But dental hygiene appointments go far beyond just cleaning your teeth. They play a vital role in maintaining your overall health. Here’s how:
- Prevent gum disease: a common yet often silent condition that can cause gum recession, bone loss, and even tooth loss if left untreated
- Catch early signs of trouble: cavities, infections, and even oral cancer are easier to treat before they become painful or complex
- Freshen breath and brighten smiles: buildup and stains which can’t be fixed by brushing at home can be professionally removed
- Support your whole-body health: Poor oral health has been linked to systemic issues like heart disease, diabetes, and respiratory infections

Rather than seeing your dental visit as just another task, think of it as a vital check-in for your health. It’s a proactive step that helps you stay ahead of potential problems and feel confident in your smile. This is simple yet powerful care which protects your body from the inside out.
Your dental hygiene appointment in 8 steps
A typical dental hygiene visit takes about 30 to 60 minutes, depending on your oral health needs. Here’s a step-by-step breakdown of what happens:
Your hygienist will start by checking in on your general health and updating your medical history. Any new medications, recent illnesses, or health conditions, like diabetes or pregnancy, can affect your mouth, so it’s important to share even seemingly unrelated details.
They may also ask about sensitivity, bleeding gums, dry mouth, or any concerns you’ve noticed.
Before cleaning begins, a visual inspection is done using a small mirror and light. The hygienist checks for:
- Inflamed or receding gums
- Signs of gum disease (like bleeding or deep pockets)
- Tooth decay
- Plaque and tartar deposits
- Early signs of oral cancer, sores, or other abnormalities
If anything concerning is found, the dentist may be brought in for a closer look.
Depending on how long it’s been since your last images, or if new symptoms are present, you might have X-rays taken. These help detect:
- Cavities between teeth
- Bone loss from gum disease
- Impacted teeth
- Cysts, abscesses, or hidden infections
Modern digital X-rays are quick, safe, and provide valuable diagnostic insight.
Oral pathogen tests help detect harmful bacteria that may be silently contributing to gum disease, decay, or even chronic disease. This test could play a role in reducing your risk of heart disease, diabetes and even Alzheimer’s disease. When you get an oral pathogen test, we determine your current oral pathogen density and review your previous history to track changes over time.
Leeming Dental is proud to be the leading clinic in Perth to offer this advanced screening. It’s an additional procedure that provides valuable insights into your oral health beyond what can be seen during a regular checkup.

If your appointment includes a comprehensive exam, the dentist will:
- Review your X-rays and the hygienist’s findings
- Examine your teeth, gums, bite, and jaw
- Look for signs of grinding, misalignment, or TMJ issues
- Discuss any treatment recommendations or questions you may have
If your dentist identifies anything that could help optimise your oral health, they’ll explain what’s happening and walk you through your options. You’ll have clear guidance and support to make the best choices for your wellbeing.
This is the heart of your hygiene visit. The goal is to thoroughly remove plaque, tartar, and surface stains to keep your gums healthy and prevent future issues.
At Leeming Dental, we offer both traditional cleaning methods and the advanced Airflow Prophylaxis Master system. Traditional tools such as manual and ultrasonic scalers effectively remove stubborn deposits, while Airflow uses a gentle stream of air, warm water, and fine powder for a more comfortable and efficient clean. Airflow is particularly suited for patients with sensitivity or dental work such as crowns, bridges, or implants, and delivers exceptional stain removal for a smoother, brighter finish.
Whether you prefer a traditional clean or the comfort of Airflow, our team will tailor your hygiene experience to your needs, helping you maintain a healthy, confident smile.
This is the heart of your hygiene visit. The goal is to thoroughly remove plaque, tartar, and surface stains from your teeth to keep your gums healthy and prevent future issues.
Many dental clinics still use traditional tools, such as manual or ultrasonic scalers, to effectively remove deposits. But some modern practices now offer Airflow Prophylaxis Master—a cutting-edge system that uses a controlled stream of air, warm water, and fine powder to clean teeth and gums more comfortably and efficiently. It’s particularly gentle for patients with sensitivity or dental works (e.g., crown, bridge, or implants) and provides excellent stain removal.
If you like your clean to be gentle and comfortable, we’ve got you covered. Leeming Dental offers both traditional methods and the advanced Airflow Prophylaxis Master system, so you can choose the approach that best suits your needs.
Your hygienist will floss between each tooth to remove any remaining debris and evaluate your gum response. They may also give you tips or demonstrate better techniques if needed.
To strengthen enamel and reduce the risk of future decay, many dental practices offer a fluoride treatment at the end of the cleaning. It’s especially beneficial for those with a history of cavities, sensitive teeth, or kids and teens with developing smiles.
Fluoride can come as a varnish, foam, or gel and takes just a few minutes to apply.
One of the most valuable parts of a hygiene visit is the professional advice you receive. Your hygienist may discuss:
- Proper brushing and flossing techniques
- The right toothbrush or flossing tools for your needs
- Lifestyle or dietary habits affecting your oral health (like snacking, smoking, or acidic drinks)
- Any early warning signs to watch for
This isn’t one-size-fits-all advice—it’s tailored to your specific needs.
Keep your smile on track between visits
Lock in the benefits of your cleaning by following these daily habits:
- Brush twice a day for two minutes with fluoride toothpaste
- Floss or clean between teeth daily
- Use an antibacterial or fluoride mouthwash if recommended
- Limit sugary and acidic foods and drinks
- Stay hydrated and avoid smoking
- Schedule checkups every 6 months—or as advised by your dental team
Clean teeth, clear conscience
A hygiene appointment does more than polish your teeth. It protects your health, your comfort, and your confidence for years to come. These visits catch problems early, prevent costly treatment later, and keep your mouth and body working in harmony.
When you stay consistent with your hygiene appointments, you can skip ahead of issues before they start. This keeps you feeling fresh, healthy, and in control.
So when that reminder pops up, don’t grumble and push it to ‘later’. Smile your whole way to Leeming Dental knowing you’re prioritising something that truly matters — you.

























