Do not pop it! The truth about your tooth abscess
Dying to pop your tooth abscess? Don’t!
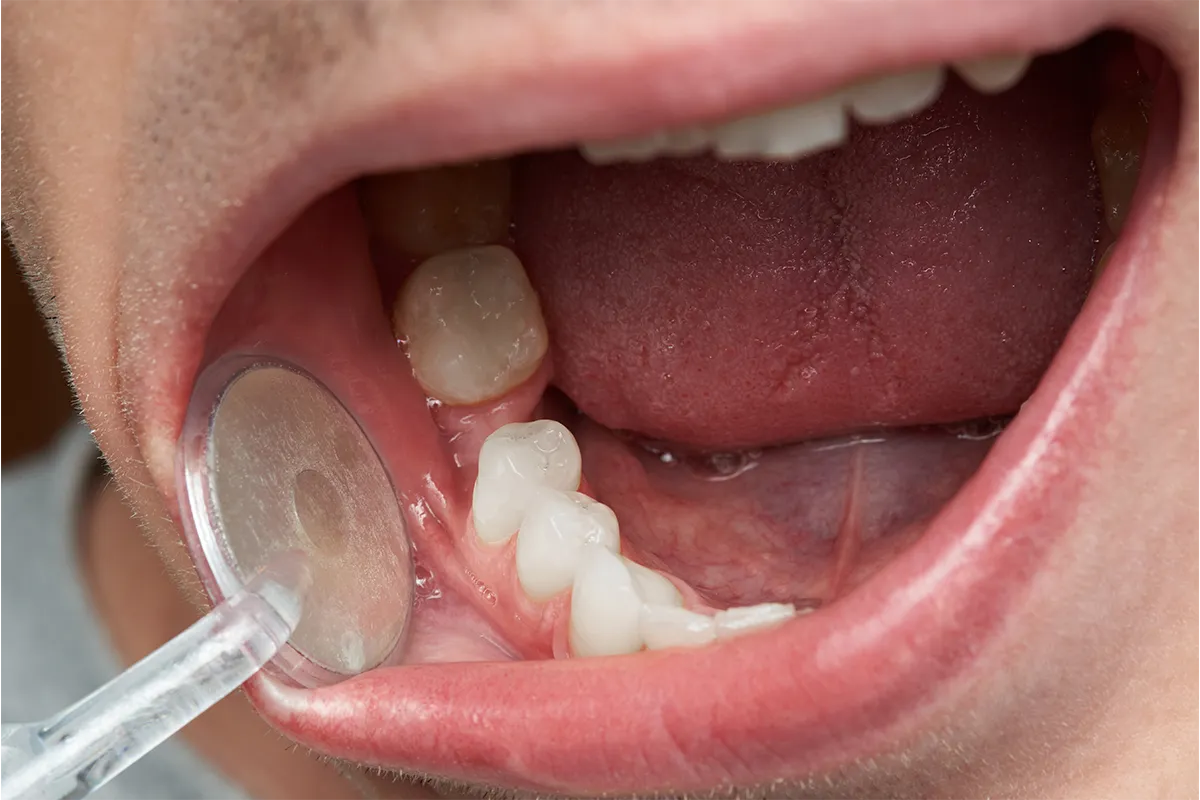
Is that a pimple inside your gum? If you’ve ever noticed a painful bump or swelling near a tooth, it’s easy to assume it’s something minor, maybe even a pimple you can pop and move on from. But hold up. That little lump isn’t a pimple at all! It’s likely a tooth abscess, and trying to handle it yourself can do far more harm than good.
A tooth abscess is your body’s way of waving a big red flag, telling you there’s an infection that needs professional care. Left untreated — or worse, tampered with — it can spread quickly and lead to serious complications. Treat this as a dental emergency and get in to see your dentist as soon as possible.
If you actually have an abscess, stop reading for a moment — call your dentist first. Good. Now that you’ve done that, let’s talk about what’s really going on. We’ll unpack what a tooth abscess is, why it forms, why you should never try to pop it, and the safest, most effective way to get rid of it for good.
What exactly is a tooth abscess?
A tooth abscess forms when bacteria cause an infection inside your tooth or gum, leading to a pocket of pus. In simple terms, it’s your body’s way of fighting back. Your immune system sends white blood cells to the area to battle the infection, which leads to a build-up of pus.
There are two main types you should know about:
Periapical abscess – develops at the tip of a tooth’s root, often due to deep decay, cracks, or trauma that allows bacteria to reach the inner pulp.
Periodontal abscess – forms in the gums beside a tooth, usually as a result of advanced gum disease or trapped food and plaque around the roots.
No matter which type you have, a tooth abscess is your body’s SOS signal — a clear sign that an infection needs professional attention before it spreads or worsens.

Why you should never pop a tooth abscess
It might be tempting, especially when the pressure builds and the pain becomes unbearable, but here’s the hard truth: popping a tooth abscess is dangerous.
What might seem like a quick fix can actually turn into a serious health risk. Here’s why:
When you try to squeeze or drain an abscess yourself, bacteria can enter your bloodstream or spread into deeper tissues of your face, jaw, or neck. In severe cases, this can lead to sepsis, a potentially life-threatening infection that affects your whole body.
Even if some pus drains out, the infection inside your tooth or gum doesn’t disappear. The abscess will almost always come back, often more painful and swollen than before. The underlying infection will still be there.
Using sharp objects like pins, needles, or even your fingers can damage your gums and surrounding tissues. You might cause bleeding or open new pathways for bacteria to spread, worsening the infection.
Every day you wait or try to “fix it” yourself gives the infection more time to grow. This can lead to tooth loss, bone damage, or the need for more complex dental procedures down the line.
The bottom line: A tooth abscess isn’t something to handle at home. Never pop or drain it yourself — see your dentist as soon as possible. They can safely relieve your pain, treat the infection at its source, and help protect your overall health.

Signs and symptoms you shouldn’t ignore
A tooth abscess doesn’t always look dramatic at first. Some start small with just a bit of gum tenderness or a dull ache, but they can escalate quickly if left untreated.
So how do you know if that swelling is something serious? Here’s what to look out for:
- Throbbing, persistent toothache that can radiate to your jaw, ear, or neck
- Swelling in the face, cheek, or jaw
- Red, shiny, or swollen gums near the affected tooth
- A small bump or pimple on the gum (which may release pus or fluid)
- Sensitivity to hot, cold, or pressure when chewing
- Tender or swollen lymph nodes in the neck or under the jaw
- Bad taste in the mouth or foul-smelling breath
- Difficulty opening your mouth, swallowing, or speaking comfortably
- Fever or general feeling of being unwell (fatigue, malaise)
If you experience any of these symptoms, especially if the swelling spreads or you start to feel unwell, see your dentist urgently or go to your nearest emergency department. Prompt treatment is crucial to stop the infection from spreading and to relieve your pain safely.
How dentists treat a tooth abscess
Thankfully, a tooth abscess is treatable, and with the right dental care, you can recover fully and get back to feeling comfortable again.
Your dentist’s main goal is to remove the source of infection, ease your pain, and prevent it from coming back. Depending on your situation, treatment may involve:

- Draining the abscess safely – Your dentist may make a small incision to release the pus and clean the area, easing the pressure and discomfort.
- Prescribing antibiotics – To control the infection and stop it from spreading to nearby tissues.
- Performing root canal therapy – If the infection has reached the inner pulp, your dentist can clean, disinfect, and seal the tooth to save it.
- Extracting the tooth – In severe cases, when a tooth is too damaged to restore, removing it may be the safest option.
Using modern tools such as digital X-rays, your dentist can pinpoint the source of infection precisely. You really can’t safely do even a fraction of this at home, but with prompt, professional care, most patients feel relief within days and are back to normal before they know it.
How to relieve the pain (while waiting for treatment)
If you can’t see your dentist straight away, there are a few things you can do to manage the pain and swelling safely at home. This is just until you get proper treatment, so please don’t mistake this for a treatment regime. It’s just a few steps to minimise trouble until your dental appointment.
Try these simple steps:
Rinse gently with warm saltwater. This helps keep the area clean and can provide mild relief from discomfort. Avoid vigorous swishing — gentle is best.
Take over-the-counter pain relief, such as ibuprofen or paracetamol, following the directions on the label. These can help ease the pain and reduce inflammation.
Avoid very hot, cold, or sugary foods and drinks. These can irritate the tooth or trigger sharp pain. Stick to softer, neutral-temperature foods until you’re treated.
Keep your head elevated when resting. Lying flat can increase pressure and make the pain throb more, so try propping yourself up slightly when you sleep.
And one important note: don’t apply heat or try to drain the abscess yourself. Both can make the infection spread faster and cause more harm than good.
These tips can help you stay comfortable for the moment, but they’re not a cure. The only way to truly stop the infection is with professional dental care.

Using modern tools such as digital X-rays, your dentist can pinpoint the source of infection precisely. You really can’t safely do even a fraction of this at home, but with prompt, professional care, most patients feel relief within days and are back to normal before they know it.
Prevention is the best way to protect your smile
The truth is, most tooth abscesses don’t start out as big problems. They often begin with something small like a bit of decay, a missed brushing session, or an untreated cavity. Over time, those little issues can snowball into a painful infection.
The best part is that most abscesses are completely preventable with simple, consistent oral care and regular dental visits.
Here’s how to keep your teeth and gums healthy:
- Brush twice a day with fluoride toothpaste to remove plaque and strengthen your enamel.
- Clean between your teeth daily using floss or interdental brushes to get rid of food and bacteria your toothbrush can’t reach.
- See your dentist regularly for check-ups and professional cleans — early detection can stop small problems from turning into major ones.
- Treat cavities, chips, or gum issues early to prevent bacteria from finding their way deeper into your tooth or gum tissue.
- Eat a balanced diet and go easy on sugary snacks or drinks, which can feed the bacteria that cause decay.
Keeping up with these habits doesn’t just protect you from abscesses — it helps you maintain a healthy, confident smile for life.
Got a swollen gum? Get it checked!
Tooth abscesses can be painful and worrying. It might be tempting to handle it yourself, but this isn’t a DIY project — let your dentist take care of it.
Your dentist has the right tools, training, and gentle touch to relieve your pain safely and treat the infection at its source.
If you notice swelling, tenderness, or an unusual lump in your mouth, book an appointment as soon as possible. Prompt treatment and good oral hygiene habits can stop infections and other issues before they start, so your teeth and gums stay healthy today and far into the years ahead.