The highest risk factors for tooth decay in children
Poor oral care and hygiene can lead to toothache and pain, with child tooth decay being the most prevalent oral condition among Australian children today. Approximately 42% of children aged 5 to 10 years old have experienced tooth cavities. While there are a range of socio-economic factors – including social, economic, cultural and environmental factors – affecting the oral health of Aussie kids, tooth decay is basically caused by accumulations of pathogenic oral bacteria.
The type of oral bacteria that cause tooth decay feed on food residue left on teeth after eating refined carbohydrate sugars and starches. These include soft drinks, dried fruits, candy, cake, cookies, fruit drinks, cereals and sweet breads. Oral bacteria metabolise these carbohydrates and produce bacterial acids. As more bacteria and acid is produced, it combines with saliva to form sticky bacterial plaque which spreads over tooth chewing surfaces and the gum line.
Over time, the bacterial acid damages tooth enamel. Once the bacterial acid penetrates the tooth enamel, it starts to damage the dentine inner layer inside the tooth to cause a cavity.
Risk factors for child tooth decay
The factors that significantly increase the risk of a child experiencing tooth decay include:
- High levels of pathogenic oral bacteria causing tooth decay, including Streptococcus Mutans (S. Mutans) and Lactobacillus spp., which are present during cavity onset and development.
- A diet high in sugars and starches, especially sweet drinks.
- Non-fluoridated home water supply.
- Poor oral care and hygiene.
- Reduced saliva flow.
- Acidic or low pH saliva.
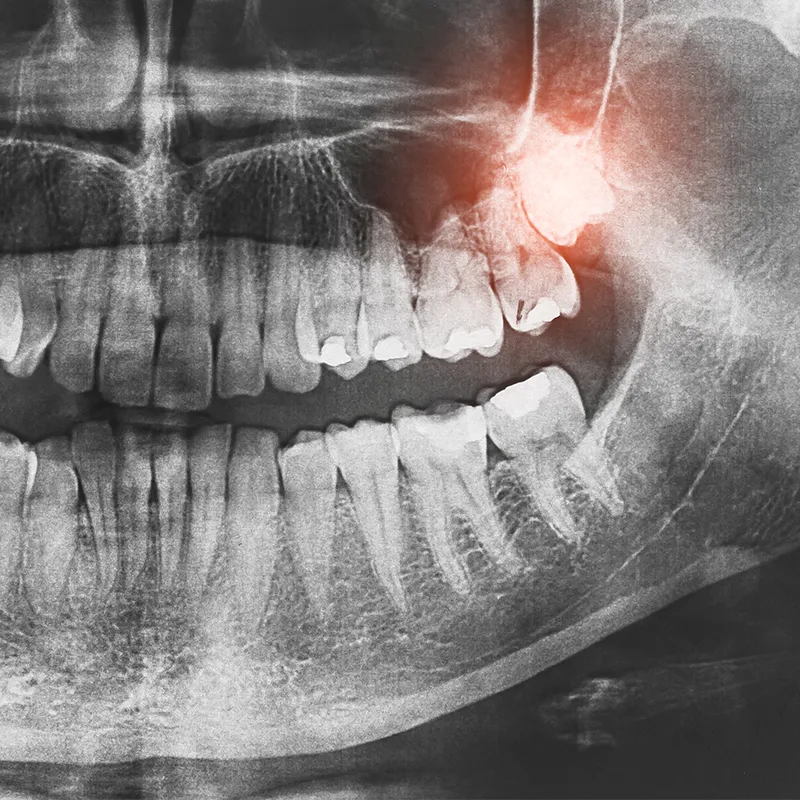
Signs & symptoms of child tooth decay
Keep in mind that children may not even experience any symptoms of tooth decay until a dental visit. So, late detection of tooth decay is also a risk factor. Early signs and symptoms of tooth decay to look out for include:
- Chalky white spots on tooth enamel show decalcification.
- Early cavities have a light brown colour.
- Deepening cavities have a dark brown or black colour.
- Toothache and pain.
- Sensitivity to food and temperature.